If you’re experiencing anxiety, it may feel as though you’re stuck in overdrive: racing thoughts, muscle tensions, and palpitations can occur in the face of small stressors, or even when the stressors are long gone. You may have been frustrated after finding that meditation, yoga, and even talk therapy couldn’t fully address your symptoms. Enduring anxiety on a regular basis can be exhausting and make you feel out of control.
What If We Could Use Technology to Calm the Overactive or Anxious Brain?
An emerging group of clinicians, including myself, have been doing just this with neurofeedback, an innovative and non-drug treatment approach that uses real-time EEG to provide the brain with information so that it can self-correct and better regulate in the face of everyday stressors.
Neurofeedback is one of a group of new brain-based therapies that encourage neuroplasticity and go beyond talk therapy. For a long time, scientists saw the brain as a hard-wired machine. But with modern research, we now know that the brain can regenerate and create new patterns of activity. Neurofeedback encourages the brain to be more flexible and to develop healthier patterns.
How Does Neurofeedback Work?
For a more detailed reading, please refer to our website on the nuances of neurofeedback training. In a nutshell though, this is how it works:
During a neurofeedback therapy session, the clinician uses an EEG to observe brainwave activity in addition to talking to patients about their feelings and symptoms. This brainwave activity is regarded as a biological marker that provides information about what may be underlying the symptoms of anxiety and other brain-based conditions. These waves vary in speed and are associated with different activities, from problem-solving to sleep. Many patients with anxiety have elevated levels of fast beta waves, which can contribute to feelings of fear, insecurity, and panic.
Neurofeedback can help reduce these beta waves, while promoting alpha waves associated with relaxation and meditation. When a patient’s brainwave activity moves into a healthier state, the brain is rewarded with a pleasant video and uplifting music or tone. This type of training is known as operant conditioning and is similar to how we would reward positive behavior when training an animal. Our brains, just like animals, are constantly seeking rewards. During a single neurofeedback session, the brain is given multiple opportunities to self-correct and be rewarded.
HPA Axis: The Body’s Stress Response System
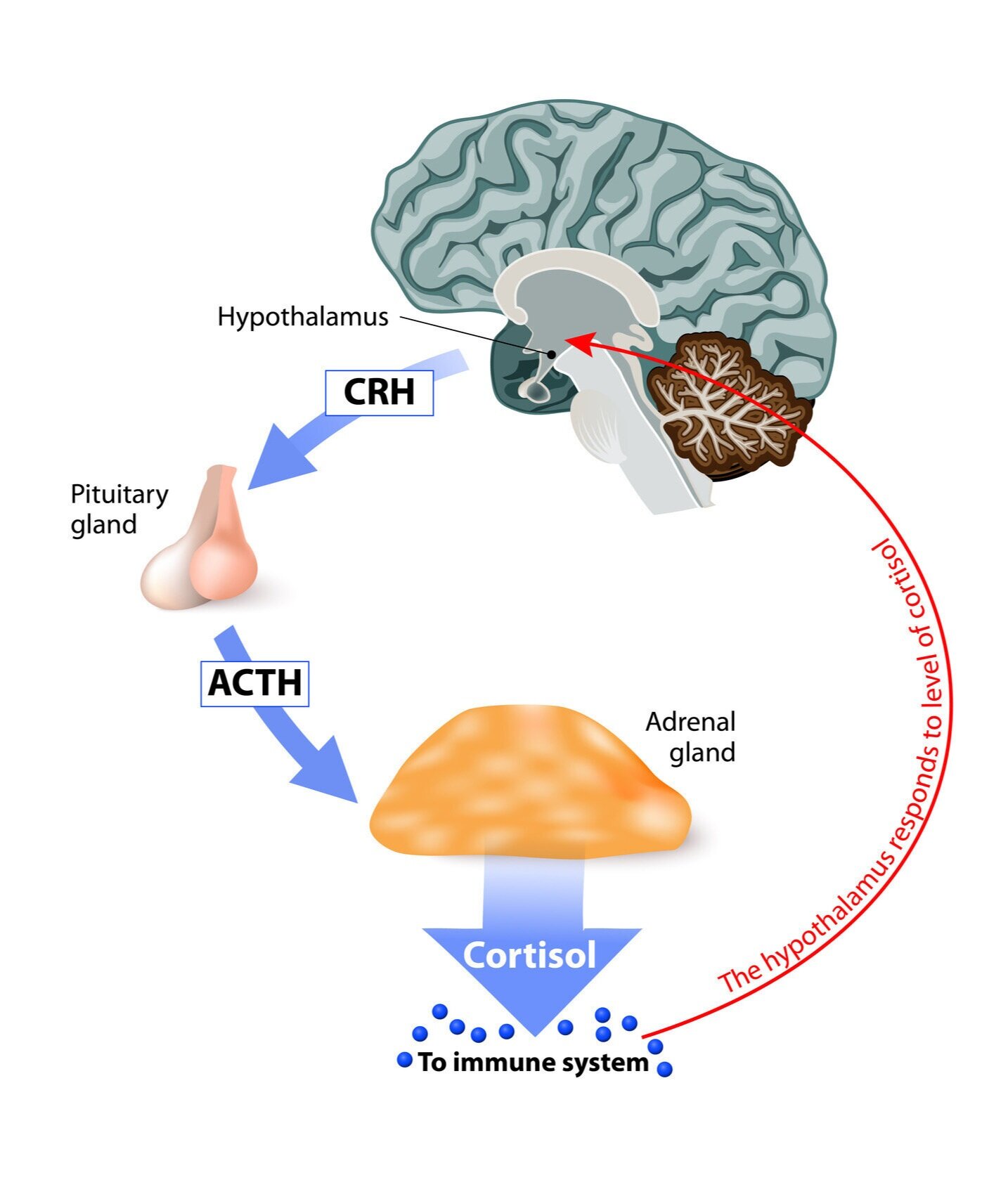
Before we look more closely at how neurofeedback can help with anxiety, let’s discuss the brain and body’s stress response system.
Our body is equipped with a central stress response system, or the HPA axis (the hypothalamic- pituitary-adrenal axis). When the brain first detects danger, it sends an alarm signal to the hypothalamus, the part of the brain that coordinates the rest of the body’s stress response. The hypothalamus then sends a signal to the pituitary gland in the brain, which produces ACTH, a hormone that travels to the adrenal glands, which then increases levels of cortisol in the blood during times of stress. We’ve all heard of cortisol, the stress hormone that puts us into ‘fight or flight’ mode.
But that’s just half of the story. The hypothalamus in the brain also puts the nervous system on alert. This is what causes someone’s breathing to change, heart rate to spike, body temperature to heat up, and pulse to speed up. The nervous system also has a complementary branch, referred to as the parasympathetic branch, which does the opposite and calms the body and mind.
What Happens to the Stress Response System in Anxiety?
The stress response is meant to be a short-term state in the face of a perceived danger, providing just enough time to help you react and escape. In anxiety disorders, however, the stress response system and HPA axis can become dysregulated.
You can think of the HPA axis as a thermostat in a house. If the thermostat is set too high, the body can become overwhelmed and over-responsive. For example, in some anxiety disorders, elevated levels of cortisol for extended periods of time can lead to a person feeling stuck in fight-or-flight mode long after the stressor is gone. On the other hand, the body can fail to respond appropriately if the thermostat is set too low. The autonomic nervous system may become less responsive and flexible, which may make it difficult to adapt to changes and stressful situations.
Slow-Wave Training: Fixing the Dysregulated Stress Response System
Within the umbrella of neurofeedback therapy is slow-wave training, or ILF/ISF (infra-low/infra-slow frequency). This, we’ve seen in our clinic, has been most helpful for anxiety, even more so than traditional neurofeedback training.
In conventional neurofeedback therapy, emphasis is placed on faster waves that are completed in one second or less. Conversely, slow-wave training focuses on the slowest brain waves that are less than .5Hz and take hours to days to complete. Research shows that these slow waves are responsible for modulating the hypothalamus and our nervous system. In other words, these slow brain waves underlie and help to regulate the set point of our HPA response system. That means they can move the set point of our body’s thermostat to a less aroused or reactive state, helping us control our response to anxiety triggers.
Many of our patients with anxiety have too much sympathetic activity in their autonomic nervous system, which indicates stress in their body. Within a single session of slow-wave ILF therapy, we can see patients experience a change in autonomic functioning as they move away from sympathetic activation and towards increased calming and parasympathetic activity, including slowed heart rate and muscle relaxation.
Our patients’ experiences mirror the results of a recent study of slow-wave training, in which researchers observed changes in objective measurements of sympathetic functioning (i.e. skin conductance, heart rate variability, and blood pressure) for patients who underwent slow-wave training. Patients who completed more conventional neurofeedback, however, did not demonstrate these changes.
What Patients Have To Say

We’ve gathered feedback from several patients after their first set of sessions. Here’s what they had to say about their experience:
“My family and friends have always told me not to worry about everything, but this is the first time I feel like it is possible and I can stop worrying.”
“After 15 minutes, I already feel so good and I can feel a change. I hope in the future I can feel this way all the time.”
“This is the first time in my life that I have been able to truly relax and enjoy the present moment.”
“I feel like I can let go of my analytic and critical brain and relax.”
While patients often start seeing temporary improvement after 3 to 5 sessions, 20 to 40 sessions are generally needed to consolidate changes for long term results.
For some patients, neurofeedback can be an alternative to psychiatric medications. In addition to neurofeedback, we found that patients see more improvements when we also look at other contributors to their anxiety, considering childhood and recent stressors along with completing functional medicine testing.
To review the research on neurofeedback for anxiety and other brain-based disorders, please refer to the bottom of our neurofeedback page.
If you are in the San Francisco Bay Area and would like to learn more about our ILF neurofeedback program, feel free to reach out to us. For others interested in finding an ILF provider near them, please visit the nationwide neurofeedback directory from EEG Info.
References
1. “How Infraslow Neurofeedback Effectively Treats Anxiety” Neurofeedback Services of New York (2018)
2. “The Effect of Infraslow Frequency Neurofeedback on Autonomic Nervous System Function in Adults with Anxiety and Related Diseases” Neuroregulation (2020)
3. “Infra-Low Frequency: A Proposed Mechanism” Brain Enhancement Centre (2011)
4. “What is Neurofeedback?” EEG Info
The information and any products mentioned in this article are not intended to diagnose, treat, cure, or prevent any disease. The information provided is for educational purposes only and not intended to replace the relationships with your physician(s). Before initiating any conventional or integrative treatments, please first consult with a licensed medical provider. Please review references cited at the end of article for scientific support of any claims made.
Suruchi Chandra, MD
By
September 1, 2020
|